- Adult Heart DiseaseDiseases of the arteries, valves, and aorta, as well as cardiac rhythm disturbances
- Pediatric and Congenital Heart DiseaseHeart abnormalities that are present at birth in children, as well as in adults
- Lung, Esophageal, and Other Chest DiseasesDiseases of the lung, esophagus, and chest wall
- ProceduresCommon surgical procedures of the heart, lungs, and esophagus
- Before, During, and After SurgeryHow to prepare for and recover from your surgery

Since vaping and e-cigarettes have become more popular over the last several years, many patients—particularly during conversations about quitting smoking—have asked me, “Is vaping okay?” or “Is vaping safe?”
As a thoracic surgeon who treats patients with lung and esophageal cancer, as well as lung transplant patients, my gut reaction has always been to emphatically say, “No!” But that response wasn’t based on hard evidence, as there really was no clear research to guide physicians when making recommendations related to vaping. Yes, we know that smoking has been shown to cause cancer and nicotine is a toxic substance that affects blood vessels—so both are harmful. We don’t know as much about e-cigarettes and the chemicals that are in them. However, we do know that you’re exposing yourself to all kinds of chemicals that we don’t yet understand and are likely dangerous. So it’s safe to say that vaping e-cigarettes is bad for your health.

What is vaping?
E-cigarettes consist of a cartridge, a battery, and an LED light. When turned on, the e-cigarette heats up the liquid that is in the cartridge, producing an aerosol mist or vapor, which the “smoker” inhales or “vapes.” The device heats up various flavorings, nicotine, marijuana, or other potentially harmful substances. Once any chemical is heated, it can change its shape or combine with other chemicals to form something different, and become damaging to tissues.

Nationwide outbreak of vaping-related lung injuries
Until now, there has been little research and few reported side effects from vaping, so I think most physicians (myself included) would not endorse vaping as safe, but couldn’t necessarily point to any specific reasons why it was harmful. This changed earlier in the year, and now more than 2,170 cases in 49 states of e-cigarette, or vaping, product use-associated lung injury (EVALI) have been reported to the Centers for Disease Control and Prevention (CDC); 42 deaths have been confirmed in 24 states. Most of the patients affected have been younger (13-24 years old), although the deaths have been in somewhat older patients (average age in the 50s, with a range from 17-75 years).
While it is not known exactly what has caused this epidemic, the CDC reported that the association is strongest with vaping products or fluid that contain tetrahydrocannabinol (THC), the active ingredient in marijuana. The CDC also identified Vitamin E acetate as a reason for the lung illness outbreak. This oily chemical is used as an additive in the production of e-cigarette or vaping products, and as a thickening ingredient in e-liquids. According to the CDC, vitamin E acetate usually does not cause harm when ingested as a vitamin supplement or applied to the skin. However, when vitamin E acetate is inhaled, it may interfere with normal lung functioning.
The CDC has recommended that you do not purchase any type of e-cigarette or vaping products, particularly those containing THC, off the street. While many of the products connected to this outbreak of lung injuries were likely homemade and distributed illegally, it’s important to note that the CDC investigation also involves a wide variety of brands and substances, including nicotine-only products, so ideally, you should stop vaping and smoking altogether. And, irrespective of the ongoing investigation, tobacco, e-cigarette, or vaping products should never be used by kids and young adults. I think we know that smoking and nicotine is addictive and that it takes tremendous effort to quit smoking. If you’re ready to quit, the safest strategy is to use nicotine gum and patches, or alternate methods of consuming nicotine that do not involve inhaling a heated liquid or smoke. Also, if you intend to use THC, you should not use any method that involves vaping or smoking. However, I recommend quitting both chemicals unless medically necessary, considering the real clear and present danger with vaping that has been reported nationwide.
‘Very real’ life-threatening effects of vaping
As the investigation continues, we may not know all of the causes for several more months or longer. This has highlighted for me that just because something seems safe, there is no sure way of knowing, particularly if it involves inhaling something other than air.
In my role as a lung transplant surgeon, I see many patients who have acute decline in lung function and need to be urgently put on the transplant waiting list or they need a machine to breath and are transplanted while being kept alive with a lot of mechanical support. These patients would certainly tell you that you should do whatever it takes to avoid having this life-saving surgery.
As I was preparing this article, physicians in Detroit, Michigan, reported performing a double lung transplant on a 17-year-old patient with EVALI, very likely the first of more to come. Doctors said the patient’s lungs were scarred, stiffened, pocked with dead spots, and extremely inflamed. On a scan before the surgery, the boy’s chest appeared almost empty, as if the lungs had vanished. The lungs were not visible because they were not working and there was no air. Without the transplant, the patient would have died, according to the transplant surgeons.
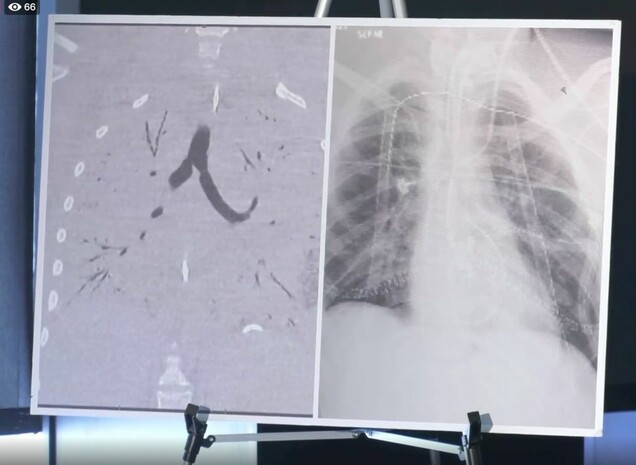
A statement from the patient’s family said, in part: “… the horrific life-threatening effects of vaping are very real! Our family could never have imagined being at the center of the largest adolescent public health crisis to face our country in decades. Within a very short period of time, our lives have been forever changed. He has gone from the typical life of a perfectly healthy 16-year-old athlete—attending high school, hanging out with friends, sailing and playing video games—to waking up intubated and with two new lungs, facing a long and painful recovery process as he struggles to regain his strength and mobility, which has been severely impacted.”
New innovations and technology will continue to become available, so it is especially important to closely evaluate their safety. Hopefully too, there will be tighter scrutiny from regulatory agencies, particularly for inhaled substances. Chemicals and their harmful effects should be analyzed extensively, in an attempt to determine the potential for infection or other damage to the lungs. Until then, my advice to you is to think twice or more before using things that could be harmful, whether smoked, eaten, or put on the skin.
The opinions expressed in this article are those of the author and do not necessarily reflect the views of The Society of Thoracic Surgeons.

