Before Lung Cancer Surgery
After being diagnosed with lung cancer, you likely will have discussed your treatment options with your medical team.
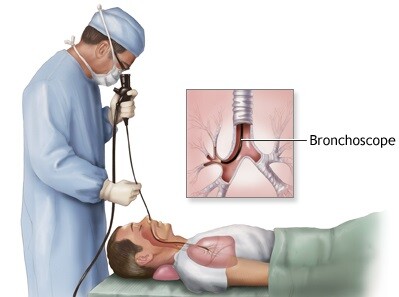
If your doctors recommend surgery, you will meet with a cardiothoracic surgeon prior to the operation. He/she will describe the operative procedure, the operative approach and incisions, the risks and benefits, and other potential options.
The more you know about your operation and what to expect before, during, and after, the smoother your recovery will be. Don't hesitate to ask questions, so that you are comfortable with your decisions going into the operation. Take plenty of notes, and consider bringing a friend or relative to the meeting, as they may be able to help you remember certain details.