- Adult Heart DiseaseDiseases of the arteries, valves, and aorta, as well as cardiac rhythm disturbances
- Pediatric and Congenital Heart DiseaseHeart abnormalities that are present at birth in children, as well as in adults
- Lung, Esophageal, and Other Chest DiseasesDiseases of the lung, esophagus, and chest wall
- ProceduresCommon surgical procedures of the heart, lungs, and esophagus
- Before, During, and After SurgeryHow to prepare for and recover from your surgery
You will be connected to many wires and tubes, including intravenous (IV) lines, one or two chest tubes, a bladder catheter, as well as monitors for your oxygen levels, heart rate, and breathing. The breathing tube that allowed the ventilator to breathe for you during surgery also is sometimes left in place while you are in recovery.
Since this can cause some anxiety, you may be given medications that make you feel drowsy until the tube is removed. Most patients don’t remember ever having the tube in place.
You will soon be transferred to your hospital room where you will continued to be closely monitored. If your surgeon prefers, you may spend a night in the intensive care unit (ICU). Your doctor will talk to your family and friends about your surgery, and let them know when they can see you. Even though you still may be asleep, your family or close friends usually will be able to visit you once the nurses have completed their initial evaluation and your vital signs are stable. Only a few visitors at a time are allowed in the ICU, so it is recommended that you limit visitors during this time and encourage everyone to visit after you’ve been transferred to a regular hospital room. Each hospital and its ICU policy is different.
After your operation, the nursing staff will constantly monitor your vital signs, chest tube drainage, breathing status, lab test results, and pain level. The anesthesia medications will be gradually weaned over the first couple of hours.
You likely will remain in the hospital for 1 to 7 days. If you underwent a minimally invasive, video-assisted procedure, your stay may be shorter compared to an open thoracotomy.
When you are awake and able to breathe on your own, the breathing tube will be removed. This is called being extubated. After the tube is removed, the nurses will make sure your breathing is normal.
Over the next few days, you will be working on recovering in the hospital. The goal is steady forward progress every day until you are comfortable and strong enough to leave the hospital. This will require that your chest tubes are removed and that your pain is under control.
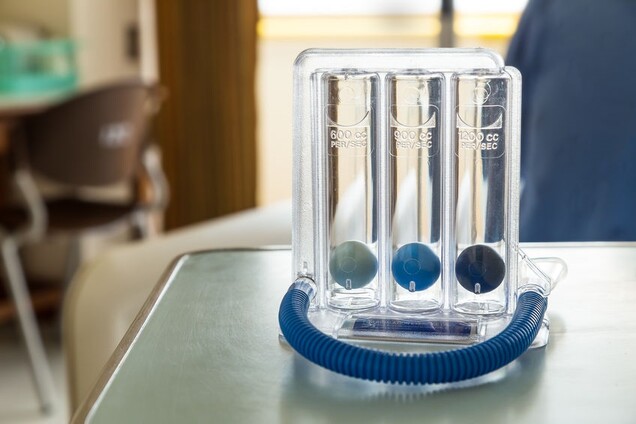
Once you feel up to it, you will be encouraged to participate in breathing exercises. A nurse or respiratory therapist will ask you to cough and assist you in the use of an incentive spirometer. This small, handheld device that you breathe into helps strengthen your respiratory muscles, improves your ability to breathe deeply, and measures how much air you can take into your lungs. You will be expected to do your breathing and coughing exercises every 1-2 hours while you’re awake.
A nurse will help you out of bed to a chair and encourage you to walk with assistance. You may not feel like being active, but early activity is important to help reduce surgical complications, such as pneumonia, blood clots in your legs, and muscle weakness. Walking every 2 hours is a good goal.
Your chest tube will be left in place until the surgeon feels that the drainage has stopped and no air is leaking. This usually occurs 2-4 days following surgery, but can vary significantly. If the chest tube needs to be left in place longer than the average amount of time, this does not mean that your recovery isn’t going as planned. Some surgeons wish to be cautious, as it’s easier to leave the tube in place a little longer than to reinsert it. After the tube is removed, the area will be covered with a bandage for at least 48 hours, unless your nurse gives you other instructions.
Your urinary catheter will be removed so that you can urinate on your own, but you may have difficulty having a bowel movement. This is due to a number of factors, including your pain medications, anesthesia medications, and not eating much. Do not be surprised if it takes 3-4 days after surgery to have a bowel movement.
Pain Management
You may experience pain or discomfort after surgery, especially in the area around the incision site. The pain can go on for quite some time, but it is usually well controlled with medication. After surgery, the strategy for pain control that your surgeon recommends for you will depend on his/her preferences and how you respond to the medications. Some surgeons like to have the anesthesiologist place a catheter near your spine (epidural) for pain control. Others prefer IV medications, allowing you to increase the dosage if you feel that you need it. In the next day or so, you’ll start taking oral pain medication instead. Your throat may feel sore due to the tube that was inserted to help you breathe during the operation. When you return home, you may be given a prescription for narcotic pain medication, or you may be able to manage your pain with nonsteroidal anti-inflammatory medications, such as ibuprofen.
Persistent pain, referred to as post-thoracotomy pain syndrome or post-pneumonectomy syndrome, can be frustrating for some people. This severe pain can occur months to years following lung cancer surgeries such as a lobectomy or pneumonectomy and may interfere with quality of life. Symptoms often include progressive shortness of breath and pain with arm movements. If you’re experiencing post-pneumonectomy or post-thoracotomy syndrome, talk to your surgeon about meeting with a pain management specialist who specializes in coping with this type of pain.
Complications
Surgery for lung cancer is a major operation and can sometimes have serious complications. Your medical team will be watching you carefully, but alert a nurse or your surgeon if you notice any concerning symptoms.
- Pneumonia: Symptoms of pneumonia, which is an infection of the lungs, include shortness of breath and fever. If you do develop this condition, it can often be treated with antibiotics; in rare cases, you may need to undergo a procedure that removes fluids from your airway. One of the keys to preventing pneumonia after lung surgery is the importance of deep breathing, coughing, and using the incentive spirometer to keep your lungs fully expanded.
- Blood clots: Long periods of laying still during and after surgery can increase your risk of blood clots forming in your legs and traveling to your lungs. Support or compression stockings are helpful at preventing clots, as is frequent walking. You also may be given medications to reduce your risk.
- Infections: You will have received antibiotics through your IV before surgery to reduce the chance that the surgical site becomes infected. Signs of an infection include redness and/or swelling around your incision.
- Fast heart rate: If you feel that your heart is racing or your chest feels tight, tell a nurse or doctor. This can sometimes occur after lung surgery, but it typically is temporary and can be treated with medication.
When you return home, you should expect to be very tired. Pace yourself and focus on the activities that take the most mental or physical energy early in the day. Cancer fatigue—described as an overwhelming sense of “whole body” tiredness—is one of the most common and frustrating symptoms you may experience following your surgery. Your fatigue will improve with time.
You also may find that it is difficult allowing people to help, but delegating some tasks and learning to accept assistance may help you recover faster. You will need help.
It is not uncommon to experience anxiety or depression after lung cancer surgery. If you are feeling especially worried or stressed, reach out to your treatment team, family, and friends. You also may want to consider joining a support group or talking with a professional counselor.
The time it takes for a return to work depends on the type of work you do, the type of surgery you had, and how fast your body heals; typically it is about 6-8 weeks after lung cancer surgery. If you feel able and if your doctor clears you, you may go back earlier, but keep in mind that you cannot drive while on narcotic pain medications, so you may need to find other arrangements. If your employer allows it, try going back part-time or with light duty as a transition back to full-time work.
Your cardiothoracic surgeon will provide you with specific guidelines, but generally, you shouldn’t lift anything heavier than 10 pounds for 2 weeks after video-assisted thoracoscopic surgery and 6-8 weeks after open surgery.
Staying Active and Eating Healthy
At home, you will be expected to walk regularly, aiming to return to at least your pre-operation level of activity within 4-6 weeks. It’s important that you don’t simply sit in bed or on the couch all day once you leave the hospital. Even if you’re only able to walk for a few minutes at a time, getting up and doing so regularly can help your recovery. As you grow stronger, try to walk for longer periods of time, but be careful not to wear yourself out. Even normal, everyday activities may be tiring for you, so make sure to stop and sit down if you start feeling overwhelmed. Try to exercise for at least 30 minutes a day.

You will probably notice some additional pain as you begin moving around more. The length of time you experience pain for and the amount of discomfort you feel will vary. Take your medications as directed and as needed, and call your physician if the medication prescribed doesn’t relieve your pain.
Your upper body may feel stiff or tight after surgery. Place a towel on your chest with a heating pad on top, or try taking a warm shower (you should not take a bath until your incision is fully healed). Talk to your physician about whether you can do some light stretching exercises to help with the tightness. Also important is to follow the instructions your health care team has provided on using the incentive spirometer at least four to six times a day.
Eating a balanced diet high in protein will help you heal after surgery. Your diet should include a healthy protein source at each meal, as well as fruits, vegetables, and whole grains. However, any previous diet restrictions that you had before surgery, such as a low-salt diet, low-cholesterol diet, or diabetic diet, likely will still be required after surgery. Do not drink alcohol, especially while you are taking pain medication, and don’t smoke. If you have questions about your diet, ask to see a dietitian.

Taking Care of Your Incision
Your medical team will explain how to care for your surgical incision once you return home. You will need to change the dressing often so that it stays clean. If you find that you need to change the dressing more than 3 times a day due to excessive fluid leaking from the incision, call your cardiothoracic surgeon. You also may have some tingling and increased sensitivity around your incision as it heals.
You may shower, but do not take baths. Gently use soap and water over your incision and pat the area dry. If shampoo or conditioner gets on the wound, just rinse it off. After a shower, pat your wound dry instead of rubbing against it. Do not soak in a pool or hot tub until your wounds are healed completely. Soaking the healing tissue could introduce bacteria from the water into your incision. It can take 4-6 weeks for your incision to fully heal.
When to Call Your Doctor
Your first appointment after surgery will be 1-3 weeks after you leave the hospital. During this appointment, your physician will discuss the pathology results with you in detail. However, don’t wait to call your cardiothoracic surgeon’s office if you have any of the following symptoms:
- Swelling, redness, or excessive drainage around your incision site
- Pain that is not helped by your medication
- Frequent nausea or vomiting
- Pain when urinating
- Inability to have a bowel movement for 4 days
- Fever 101°F or higher
- Pain or swelling in your legs or ankles
- Skin rash
The following symptoms are emergencies, so call 911 or have someone drive you to the nearest emergency room if you experience them:
- Severe headache or abdominal pain
- Sudden, sharp pain in your chest
- Coughing up bright red blood
- Sudden numbness or weakness in your arms or legs
- Shortness of breath that is not relieved by rest
- Racing heartbeat
- Fainting
For more information, read the blog, “What Patients Should Know About Life After Lung Cancer Surgery” by Leah M. Backhus, MD.
Read more about Lung Cancer.
Reviewed by: Robbin G. Cohen, MD
October 2018


