- Adult Heart DiseaseDiseases of the arteries, valves, and aorta, as well as cardiac rhythm disturbances
- Pediatric and Congenital Heart DiseaseHeart abnormalities that are present at birth in children, as well as in adults
- Lung, Esophageal, and Other Chest DiseasesDiseases of the lung, esophagus, and chest wall
- ProceduresCommon surgical procedures of the heart, lungs, and esophagus
- Before, During, and After SurgeryHow to prepare for and recover from your surgery
May 26, 2017

Endovascular stent graft repair is a minimally invasive method to treat aneurysms of the descending thoracic and abdominal aorta.
An aneurysm is a bulging, weakened area in the wall of a blood vessel that results in dilation (ballooning) of the vessel to more than twice its normal size. It can occur in blood vessels of any area of the body, including the brain, aorta, intestines, kidneys, spleen, and legs. The aorta, the largest artery in the body, is the most common location of an aneurysm.
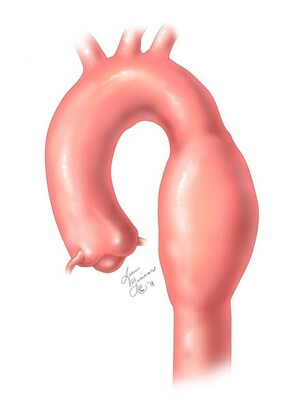
Endovascular aneurysm repair is similar to the approach used for a cardiac catheterization of the coronary arteries. It requires only small incisions in the groin or often no incision. Through the blood vessels (most commonly in the femoral artery), the surgeon inserts long tubes called catheters into the affected area of the aorta under x-ray guidance; the weakened area of the blood vessel is treated by inserting a tube, called a stent graft.
The stent graft is a fabric tube that is delivered through the catheter in a collapsed state and then expanded at the site of the aneurysm. The tube replaces and reinforces the diseased aortic wall, ensuring continuation of blood flow while preventing further expansion of the aorta, aortic rupture (bursting), and/or aortic dissection (a tear).
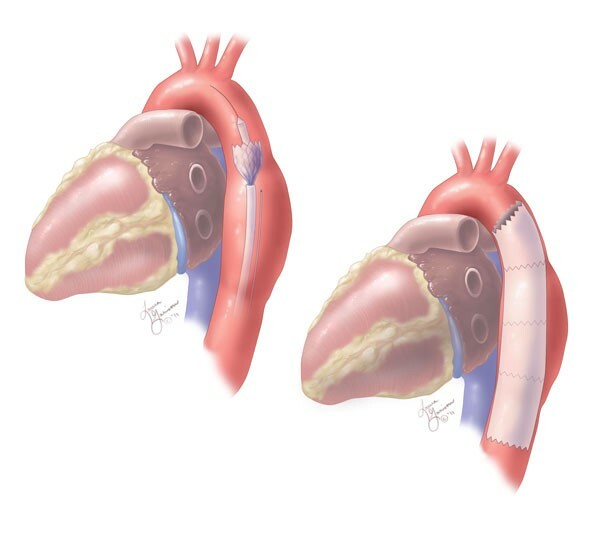
When should an aortic aneurysm be fixed?
Aneurysms are often discovered incidentally while patients are being tested for other reasons. Most people with aortic aneurysms experience no symptoms unless the aneurysm is extremely large or an aortic dissection occurs. In most cases, endovascular aneurysm repair is performed to prevent aortic dissection or rupture of the aorta. These events may lead to immediate death if they occur.
The risk of dissection and rupture increases as the aneurysm grows. The risk of aortic rupture is less than 1% annually when the aneurysm is 4 cm in size. It is more than 5% per year at 5 cm and more than 10% per year when the aneurysm is larger than 6 cm. Given the significant risk of rupture after an aortic aneurysm reaches 5-6 cm, treatment usually is recommended when it is 6 cm or larger; however, this threshold may vary for each patient based on other factors, such as vascular conditions or the need for additional surgery.
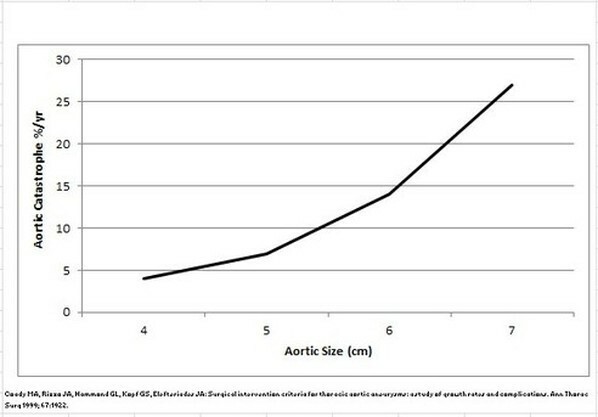
Specific treatment is determined based on patient age and preference, signs and symptoms, overall health status, medical history, and tolerance of specific medications. Other factors include the size and extent of the aneurysm, procedures or therapies, and expectations based on disease course.
Is endovascular aneurysm repair the best option?
An endovascular stent graft repair is used to treat most aneurysms of the descending thoracic and abdominal aorta. The potential benefits of the procedure, compared to traditional open surgery, include a shorter hospital stay and a more rapid recovery.
However, not all aneurysms can be repaired using an endovascular stent graft or by an endovascular approach alone. Sometimes, aortic aneurysms may require traditional open surgery or “hybrid procedures.” Hybrid methods use both endovascular stenting along with open surgery. The hybrid procedures ensure the benefits of both while minimizing the limitations and related risks of using either alone.
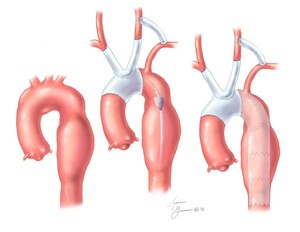
Complications associated with endovascular stent grafting include:
- Blood leakages around the stent graft
- Movement of the graft from its original site of placement
- Infection
- Blockage of blood flow through the stent graft to major organs
- Rupture of the aneurysm or aorta
What is life like after endovascular stent graft repair?
Given the less invasive nature of endovascular stent graft repair, recovery is often very quick and patients face very few limitations.
Specific after-care should be directed by a physician. However, in general, patients should:
- Monitor and keep their blood pressure well controlled
- Continue low-impact exercises (e.g., brisk walking) and avoid high-impact exercise that can significantly increase blood pressure (e.g., weight training)
- Not smoke after the procedure or take steps to quit smoking
- Wear a seat belt, since it reduces the risk of traumatic injury to the chest area
Visit Thoracic Aortic Aneurysm for more information.
Read more blogs here.
The opinions expressed in this article are those of the author and do not necessarily reflect the views of The Society of Thoracic Surgeons.

