- Adult Heart DiseaseDiseases of the arteries, valves, and aorta, as well as cardiac rhythm disturbances
- Pediatric and Congenital Heart DiseaseHeart abnormalities that are present at birth in children, as well as in adults
- Lung, Esophageal, and Other Chest DiseasesDiseases of the lung, esophagus, and chest wall
- ProceduresCommon surgical procedures of the heart, lungs, and esophagus
- Before, During, and After SurgeryHow to prepare for and recover from your surgery
July 16, 2019

Technology has transformed many areas in medicine, improving safety and efficiency. For very complex cardiac surgery — such as in babies born with heart defects (congenital heart disease) or newer surgical options for valve disease treatment with catheters and wires called transcatheter valve surgery — 3D models have helped make operations that were not possible 10 years ago routine today.
Cardiac surgery is often compared to flying an airplane. Although the similarities may not be apparent at first, the comparison actually makes a lot of sense. Cardiac surgeons and pilots train for many years before starting their careers. Both function in high-stress environments with teams of people and many variables that can impact success. The airline industry has used simulation to train and test pilots and ensure passenger safety. While simulation has started being utilized in cardiac surgery, nothing compares to actually performing the operation.
Many times, imaging such as echocardiograms (ultrasound), angiography (special x-rays using dye to visualize the heart and vessels), or computed tomography scans are used to better understand a patient’s anatomy. Although these types of diagnostic tests are helpful in identifying the problem, they aren’t able to determine how the problem can be fixed. That is where 3D modeling comes in.
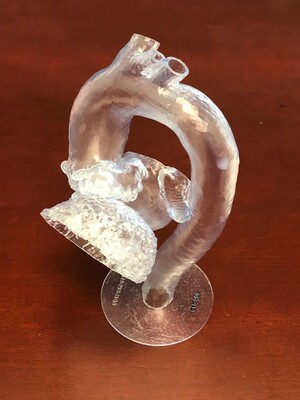
With advanced 3D imaging, we can recreate the patient’s anatomy and practice the entire operation. For structural heart surgeries, like transcatheter aortic valve replacement, this is often accomplished with a computer-generated 3D image, where the exact anatomy — from the damaged valve in the heart all the way to the vessel in the leg where the catheter may be inserted — can be reconstructed in order to plan a safe operation. The specific valve that is best for that individual patient can be selected before entering the operating room. This technology also can be helpful in congenital heart surgery. In some cases, the baby’s anatomy may be abnormal and so complex that it is difficult to repair the tiny heart during surgery. A 3D model can be created so that the heart can be evaluated before the operation.
In addition, images from the ultrasound, x-rays, and other scans can be employed to create 3D printed models that can be used for simulating the procedure. In fact, currently under investigation are many new devices that print the patient’s heart and vessels in a 3D model, allowing the surgeon and team to practice the procedure multiple times and perfect the technique. This preparation may make the actual operation safer.
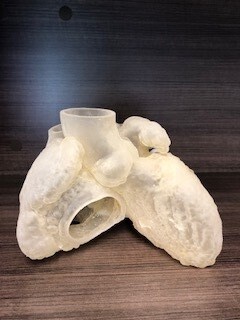
With 3D modeling and printing, the surgical team is better prepared for challenges in the operating room — similar to how pilots in simulators practice flying in bad weather or a crash landing. If you were on an airplane, you would not want the first time your pilot flew in the snow to be the day you were on the plane. Cardiac surgeons can now use 3D modeling technology to simulate complex operations, making the seemingly impossible possible.
The opinions expressed in this article are those of the authors and do not necessarily reflect the views of The Society of Thoracic Surgeons.

