- Adult Heart DiseaseDiseases of the arteries, valves, and aorta, as well as cardiac rhythm disturbances
- Pediatric and Congenital Heart DiseaseHeart abnormalities that are present at birth in children, as well as in adults
- Lung, Esophageal, and Other Chest DiseasesDiseases of the lung, esophagus, and chest wall
- ProceduresCommon surgical procedures of the heart, lungs, and esophagus
- Before, During, and After SurgeryHow to prepare for and recover from your surgery
July 21, 2017

As a surgeon, I have inside information on how a hospital works and how patients experience various tests and procedures; however, when I became a heart surgery patient, I had to ask myself several very basic questions: How much pain would I have? How long would I have to be off work? Could I have complications that might hinder or possibly end my career or even end my life? How long would it be until I felt fully restored and able to resume my life as it was before the operation?
In preparation, I created a realistic narrative to guide and manage my expectations. I relied upon medical, family, and spiritual advice. My internist, cardiologist, and my cardiothoracic surgeon were superb in helping me prepare for my recovery. Each doctor was aware of my work ethic and drive. They understood that I wanted to recover and get back to work as quickly as possible after the operation.
Dr. David Ott, of the Texas Heart Institute, was the surgeon chosen by my cardiologist and me. I first learned of Dr. Ott’s excellent reputation in the late 1980s when I was a resident in general surgery at The University of Texas Medical Branch at Galveston (UTMB). During my pediatric surgery residency training at Texas Children’s Hospital, I received further affirmation of his abilities when working with him on a case to separate the hearts of conjoined twins.
I have a congenitally abnormal aortic valve, and I had been getting echocardiograms every 3 years for about 10 years. When the serial echocardiograms and my cardiologist determined that the time for my valve replacement had come, I knew that the best opportunity for my complete and rapid recovery was for the operation to be performed by Dr. Ott.
Before my operation
My preoperative visit with the cardiologist, anesthesiologist, and perioperative nursing team helped me prepare for the day of surgery and immediately after. I also was helped by the experience of my uncle who underwent a successful emergency coronary artery bypass grafting (CABG) surgery. He told me every detail of what to expect from the chest incision to the resumption of exercise after operation. Finally, I asked for and received the prayers of my family, friends, and church.
The day of my operation
On the day of operation, my high school sweetheart and wife, Pamela, was with me until I went into the operating room. She remained with me step by step in the recovery process.
I remember the preoperative area; however, I don’t remember going into the operating room. My earliest recall after leaving the preoperative area is waking up in the postoperative intensive care unit with my arms restrained and the endotracheal tube in place. I had been told to expect the restraints to prevent the unplanned pulling of tubes, monitors, and wires. I was unable to speak, but I felt reassured by my nurse, who was very attentive, that I could communicate with him. He encouraged me to use the pain relief or patient-controlled analgesia (PCA) to manage my pain. I had decided after the preoperative anesthesia visit to optimize the use of the PCA, so every time I woke up, I pushed the button.
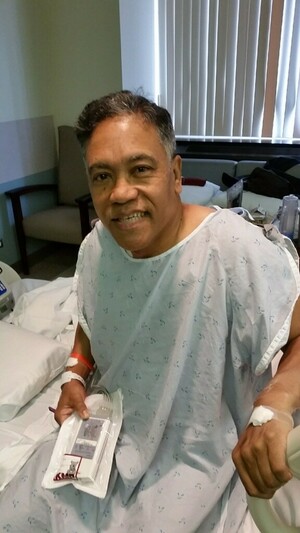
How I felt after surgery
I did not experience any chest wall pain for 3 days after the operation. And then, I only felt pain because I erroneously thought that I could go without pain relief. I had refused the hydrocodone because it made me dizzy and nauseous. On that third postoperative night, I woke up with pretty good chest wall pain; however, this pain was completely relieved with a dose of intravenous morphine and Tylenol with codeine in scheduled doses. I did not experience any more pain until 2 weeks after the operation, when I was transitioning off of the Tylenol with codeine to regular Tylenol.
My urinary catheter that was placed during the operation was removed the morning after. I experienced severe pain with urination on the first several attempts, but, this eventually passed. I needed assistance with sitting up, turning in bed, walking, and getting out of bed to go to the bathroom. I had been told to ask for and expect this help. Again, the nurses were very attentive and informative. On the first postoperative day, I sat in bed and in a chair.
My cardiologist delayed my discharge to manage episodes of atrial fibrillation for which I did not experience any symptoms. I would go home after more monitoring and administration of an oral anticoagulant that I would take for 3 weeks after the operation and that would reduce the risk of stroke.
“Stepping” out
While in the hospital, I was very cooperative with the requests to get out of bed and walk. In preparation for the operation, I had walked daily for several months and monitored my steps with a Fitbit. During those months, I walked and jogged an average of about 60,000 steps per week. The week before the operation, I recorded 72,389 steps.
Dr. Ott and I had also discussed postoperative cardiac rehabilitation, and he simply said that I could walk as much as I could. The week after discharge from the hospital I recorded 84,632 steps, with 13,294 steps logged exactly 1 week after surgery. For the first year after the operation, I averaged 60,000 steps per week. On the advice of my cardiologist, I tried not to jog or run for 3 months.
My diagnosis of severe aortic valve stenosis
One could reasonably ask why I needed a heart valve replacement if I could exercise so much to prepare for the operation. I had similar questions when my cardiologist informed me that my aortic valve stenosis had become severe and that I needed to have my diseased aortic valve replaced. I asked him exactly what “severe” really meant. It sounded excessive, especially since I had no heart symptoms. I could work as a busy pediatric surgeon day and night, walk stairs, exercise on a treadmill, mow my lawn, etc. I could do all of these activities without shortness of breath, fainting, or chest pain. If I wasn’t having any problems, could the condition of my valve be that severe? Furthermore, I asked, “How can an operation on me, a patient with no symptoms, actually make me better?”
Sometimes and as commonly surmised, it is what you don’t know that can be your downfall. My cardiologist explained that “severe” aortic valve classification is based on the cross-sectional area of the narrowed valve opening and not on the patient’s symptoms. My echocardiograms showed the valve opening was getting narrower.
I did not want my aortic valve status to become critical. I think my father’s valve became critical when he was about 50 years old. He had a murmur like mine and had a nonfatal “heart attack” and stroke in the early 1960s when I was 6 years old. Doctors later confirmed that he had aortic stenosis but no coronary artery disease. He had to retire from active duty in the United States Army after 20 years. I did not want this to happen to me. He survived until he was 79 years old.
I realized that syncope (fainting), heart attack, or stroke could happen to me if my diseased valve advanced to “critical” aortic stenosis. I did not want any of these adverse events to hasten my death or early retirement from my career. I am blessed to love what I do and want to continue to do it for a long time. Therefore, I had to get the operation done and done right to assure my complete recovery.

Complete recovery
Complete recovery for me followed what was outlined by my cardiologist and cardiac surgeon. I was off of all pain medications 4 weeks after surgery; I was driving 6 weeks postoperatively; and I returned to work 8 weeks after the operation. I had a sense of vulnerability of the chest incision that lasted up to 1 year; however, I had no movement or slipping of the sternotomy incision.
At nearly 1.5 years after operation, I consider myself completely healed and recovered. I no longer live with the threat of complications from aortic stenosis. At 61 years old, I have gained a new lease on life. My recovery from heart surgery was what I expected and followed the narrative that I had created with the advice and support of my family, friends, doctors, and pastor. I did my part and the medical team did theirs to get this operation right. My recovery was a team effort made more complete by my spiritual belief.
Learn more about Aortic Valve Disease.
The opinions expressed in this article are those of the author and do not necessarily reflect the views of The Society of Thoracic Surgeons.

