- Adult Heart DiseaseDiseases of the arteries, valves, and aorta, as well as cardiac rhythm disturbances
- Pediatric and Congenital Heart DiseaseHeart abnormalities that are present at birth in children, as well as in adults
- Lung, Esophageal, and Other Chest DiseasesDiseases of the lung, esophagus, and chest wall
- ProceduresCommon surgical procedures of the heart, lungs, and esophagus
- Before, During, and After SurgeryHow to prepare for and recover from your surgery
Part Two: When to Listen
This story is continued from Part One: When to Slow Down.
Finally, in December, I made an appointment to see my doctor.
The night before my appointment, my wife and I were hanging some Christmas decorations outside on a tree. I told her I had to go in the house because I wasn’t feeling good. She asked if I wanted to go to the hospital, but I said no, I have an appointment with my doctor tomorrow and that should be fine.
At my doctor’s visit he told me to schedule some tests but that if I had any more of these chest pain incidents, I should go to the emergency room immediately. I said OK, no problem.
Well … being the hardheaded person that I am, I really didn’t follow his direction.
That evening I had another chest pain incident, followed by one the next night as well as one in the morning on Thursday, December 17. The morning incident scared me. I came in from putting the garbage cans out at the curb to a pain that made me think, If this is not a heart attack, I don’t ever want to experience one.
I calmed myself down, the pain went away, and I went to work. I know this sounds crazy—and it is crazy that I let it get to this point.
Later that evening, I was coming back from walking the dog and I had yet another chest pain incident. I went into the house, but something told me, Don’t go sit on the couch—go upstairs. So I went upstairs and was bent over in pain, and my wife asked me, “What is going on?”
I told her, “Everything is OK; I just need about 15 minutes, and it will go away.” She told me I was crazy and that she was calling 911. I told her don’t bother—just take me to the hospital.
We walked into Edwards hospital in Naperville and they immediately started to run some tests. They said I had some blockage and that they would keep me overnight, and a cardiologist would see me in the morning. I remember thinking to myself, Oh, great—now look what’s happened.
The cardiologist came in on Friday morning and told me I was going to have a procedure done to put a stent in one of my arteries that was clogged. He said it’s a standard procedure and then I would be home tomorrow, Saturday. I went into the procedure, which he said would take a couple of hours with recovery.
Fifteen minutes into the procedure, the cardiologist went to see my wife in the waiting room. She asked him what the matter was, and he said that there was too much blockage and I needed surgery.
I was back in the room at the hospital that afternoon. The surgeon came in and talked to me about what I needed to have done and how I was pretty sick. He said surgery would happen, but it might have to be Monday. I asked, “Well, if it happens Monday, can I go home for the weekend?”—because I had some holiday baking to do.
He looked at me and said, “You are very sick. I am putting you in the cardiac ICU today.”
He also said that he’d talk with his team to get clearance to do the surgery the following morning, Saturday.
It was at this point I realized, This is not good. All kinds of thoughts raced through my head. My wife. Our two daughters, who were a senior in high school and a sophomore in college.
That evening and night were some of the longest hours of my life. Family and friends came to visit me and just shook their heads in disbelief.
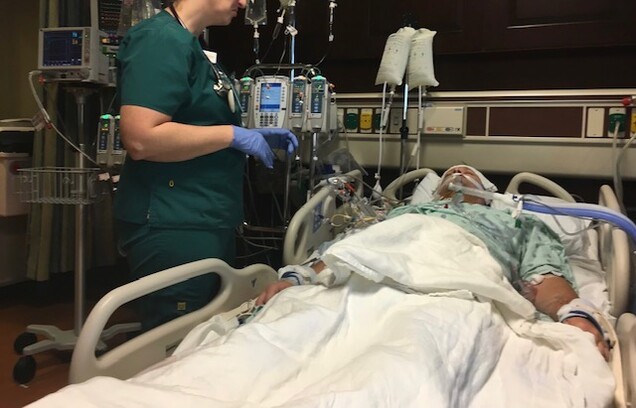
The morning of surgery was a little nerve wracking, but I guess that’s normal. My wife was her usual positive self, which made the mood easy. Five hours after surgery I was back in my hospital room. A quadruple bypass patient. All kinds of machines and tubes. it was surreal.
After some of the sedation started to wear off, the pain really started to set in. At one point my wife asked the nurse what kind of pain medicine she was giving me because it didn’t seem to be working. The nurse said that since I had declined morphine, she was giving me Tylenol.
Being a person in recovery since 1993, I’ve heard too many stories of people falling out of sobriety due to pain medicine and I didn’t want to go there. However, I realized that I really needed to follow the doctor’s direction on this.
Happy to say that my sobriety date didn’t change. I used the morphine as directed and no more.
The next day, Sunday, my surgeon came to visit me and see how I was doing. He mentioned the four arteries had been 80%, 90%, 99%, and 100% blocked. And then he said something I will never, ever forget: “My team and I find it incomprehensible that a catastrophic event hadn’t taken place.”
Dr. Bryan Foy saved my life. I will never forget him and his team for giving me the opportunity to still be here. As he turned to walk out of the room, he said, “It looks like you still have work to do.” How true that is.
My cardiologist said I could not participate in any races for the entire 2016 year. I was fine with that, as I just took my time building strength and endurance. After 12 weeks of cardiac rehab I was doing a lot better. I was able to gradually build up to running about 5 miles a day, 3 days a week, by the end of the year.
At the start of 2017, I had put on my calendar the three half marathons that I had done in the past and looked forward to getting back after it.
But you know what they say—life happens. At the end of April 2017, my wife was diagnosed with stage 3 breast cancer. It was devastating news for us, but she’s a fighter and we hit it head on. I was reminded of what my surgeon said—that I still have work to do.
Being able to help her through 16 chemo treatments in 20 weeks, followed by surgery, and then 7 weeks of daily radiation was all due to the grace of God letting me be here. I continued to run, but I just had a different perspective on life.
In 2018, I put the three half marathons on the calendar again. I approached them with a different mindset, not caring what the time was or the place. My goal was just to finish. My wife went through an excruciating trial for her breast cancer, and I was able to be a support for her. What she had gone through over the 14 months since her diagnosis was far beyond what I had gone through with my heart surgery. I would use my runs as a way to clear my head and find some peace.
2019 proved that I was mortal when it came to running. My times had slowed, and the races seemed more of an enjoyable experience rather than the pressure to win or beat my previous times.
And I was totally fine with this. I found a new love of running again. It took a brush with death, having gone through a quadruple bypass, as well as witnessing the excruciating ordeal my wife had gone through, in order for me to be at peace with myself.
We all know what happened in 2020 with COVID and its effect on the world. I did not avoid it either, as I caught the virus twice, once in April and a second time in November. I have had residual effects with aching muscles in my legs as well as soreness in my hands, both of which are still very present to this day. Although I can only go for a three-to-four-mile jog now, even that having to walk a little after the first mile, I’m totally fine with it. At least I can get out and enjoy it.
In telling my story, I hope even one person may learn how important it is to listen to our bodies and see a professional if something is not right. I was exhibit A of how being stubborn almost cost me my life.
We all have a story. We all have had things happen to us or to those we love that affects our health. God has gifted doctors, nurses, and other health professionals with the knowledge to help all of us. I know I will take that as a hard lesson learned. I have been able to experience life happenings and places that would not have been possible but for getting a lucky break. Most importantly, time with my family. For all these blessings, I am grateful that God is in my life and allowed me to continue to be a witness of His grace.
Despite how this story sounds, I actually do not like talking about myself. I’m more of the “How are YOU doing” guy. However, I want to thank my dear friend Jen for asking me to tell my story. I apologize that it has taken a very long time to write it and I’m not one to use the word “but” in an apology so I’m just sorry for the delay. Writing this gave me a renewed gratitude for getting another chance at life.
Make today great … it’s a choice!
Mitch