- Adult Heart DiseaseDiseases of the arteries, valves, and aorta, as well as cardiac rhythm disturbances
- Pediatric and Congenital Heart DiseaseHeart abnormalities that are present at birth in children, as well as in adults
- Lung, Esophageal, and Other Chest DiseasesDiseases of the lung, esophagus, and chest wall
- ProceduresCommon surgical procedures of the heart, lungs, and esophagus
- Before, During, and After SurgeryHow to prepare for and recover from your surgery
November 21, 2016

When we think of cancer awareness and the diseases that impact women in this country, which malignancies first come to mind? Given the events that receive media attention, popularized fundraisers, and efforts to raise cancer awareness, lung cancer in women is certainly not high on the list.
It is true that lung cancer rates for women in the US are substantially lower than rates of breast cancer, and that the incidence of lung cancer for women in this country has been declining since the mid-2000s. Nonetheless, despite those statistics, there’s a very important fact that many people don’t know: lung cancer is the #1 cancer killer of women in developed countries—more than breast cancer, more than colon cancer, more than any other malignancy.
Lung cancer takes the lives of more mothers, daughters, sisters, friends than any other cancer; yet, it is overwhelmingly under recognized.
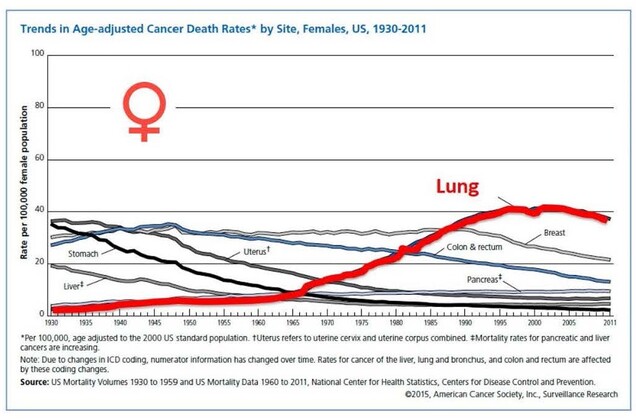
Lung cancer has been the most lethal malignancy for women in the US since 1980 (Figure). Resulting in approximately 160,000 annual deaths in this country alone, lung cancer accounts for only 13% of new cancer diagnoses, but nearly 30% of cancer lives lost. Gender differences in lung cancer mortality over time likely reflect historical differences in patterns of smoking and smoking cessation over the last 30 years.
However, not all lung cancer is caused by smoking, and, in fact, lung cancer among nonsmokers happens more often in women than men.
Not only does lung cancer claim almost twice as many lives of women in the US compared to breast cancer, there are also differences in the way that women develop lung cancer and respond to its treatment. Statistics usually lump men and women together, but for women, the chances of survival are higher at all stages of the disease. We are just beginning to learn how genetic and hormonal influences play a role in the development of lung cancer and what might explain these differences. Perhaps there are behavioral and social differences that make an impact as well.
In terms of getting diagnosed with lung cancer, women tend to be slightly younger than men, by an average of about 2 years at the time of diagnosis. This may be related to the ways that women develop lung cancer. Some studies suggest that women are more susceptible to the chemicals and carcinogens in cigarettes, causing them to develop lung cancer after fewer years of smoking.
In addition, the percentage of nonsmoking women who develop lung cancer is higher in women than in men, so there are definitely other factors besides the impact of cigarettes that determine how women develop lung cancer. A recent study showed that estrogen might promote growth of lung tumors, which could potentially account for the earlier age of diagnosis in women. Some groups of nonsmoking women, such as women of Asian descent, appear to be at particularly high risk for lung cancer. While 85% of lung cancer deaths in men are thought to be associated with smoking, this is true of only 70% of lung cancer deaths in women. Worded differently, 30% of women who die of lung cancer have never smoked.
In terms of treatment, women historically respond to a few chemotherapy medications used for lung cancer better than men, especially some targeted therapies that specifically attack cells with genetic abnormalities. When it comes to survival, women are more likely to survive lung cancer than men at all stages of the disease. This survival advantage is greatest for early staged disease, when surgical treatment of lung cancer offers a greater chance for cure in women than in men.
Lung cancer is not a disease of just men, and it is not a disease of just smokers.
It is a malignancy that is impacting the lives of men and women all around us, and it is claiming the lives of more women in this country than any other cancer. It’s time that we give it adequate attention, awareness, and research support, so that we can improve the lives of our daughters, nieces, granddaughters, and generations to come.

Read more about lung cancer.
Read more blog articles.
The opinions expressed in this article are those of the author and do not necessarily reflect the views of The Society of Thoracic Surgeons.

