- Adult Heart DiseaseDiseases of the arteries, valves, and aorta, as well as cardiac rhythm disturbances
- Pediatric and Congenital Heart DiseaseHeart abnormalities that are present at birth in children, as well as in adults
- Lung, Esophageal, and Other Chest DiseasesDiseases of the lung, esophagus, and chest wall
- ProceduresCommon surgical procedures of the heart, lungs, and esophagus
- Before, During, and After SurgeryHow to prepare for and recover from your surgery
August 18, 2020

Although the saying goes “men are from Mars, women are from Venus,” one thing both have in common is the #1 cause of death—cardiovascular disease.
1 in 4 men and 1 in 5 women die from cardiovascular disease each year. In 2017, 30.3 million adults were diagnosed with heart disease and 647,457 died from it.
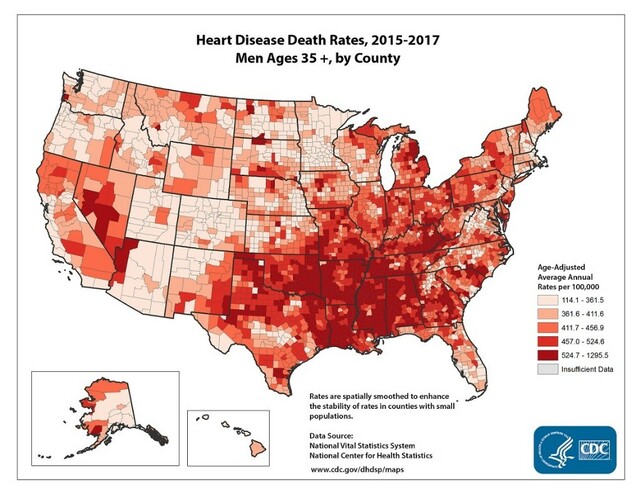
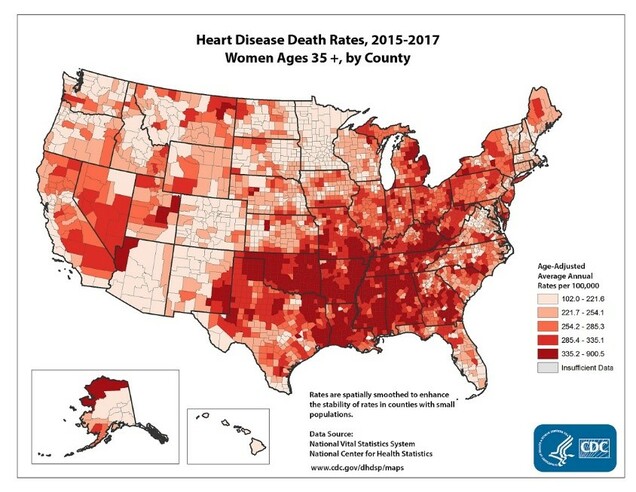
Biology and Epidemiology
The most common type of heart disease in both women and men is coronary artery disease (CAD). This is a condition where plaque builds up on the wall of the blood vessels that feed the heart. The plaque can grow slowly over time, or it can rupture suddenly leading to a major heart attack. It also is possible that the plaque will erode, leading to a clot that inhibits blood flow in the vessel.
Historically, women tend to develop heart disease later in life than men—by 7 to 10 years. This is due to the protective effects of estrogen. Around the time of menopause, changes in levels of estrogen and other steroid hormones can cause variations in blood vessels, cholesterol levels, and energy metabolism. These changes seem to contribute primarily to CAD.
Younger women are not completely without risk, however. Risk factors such as obesity, diabetes, and smoking can lead to heart disease in younger women as well. Women with diabetes tend to have worse heart-related outcomes than men.
In addition, women who develop heart disease and experience heart attacks seem to have worse long-term consequences. The reasons for these differences are still unclear and being studied. Finally, there is an increasing recognition that depression, which is more common in women, may be a risk factor for heart disease and heart-related outcomes.
The type of heart disease also can be different in men and women well. Men tend to develop disease in the main arteries that feed the heart (CAD), while women are more likely to develop disease in the smaller arteries (microvascular disease).
When plaques exist in the main arteries, they behave differently. Men are more likely to have plaque ruptures, while women more frequently have plaque erosions. Another type of heart disease—valvular heart disease—also has differences in men and women. Different valves are affected at different rates and by different disease processes. For example, mitral valve prolapse and tricuspid valve disease tend to affect women more than men.
Presentation
For many years, it was believed that heart disease was a “man’s problem.” The descriptions of a heart attack—a “crushing chest pain” and feeling like “an elephant is sitting on my chest”—were and are still true for most male patients. With time, we have come to recognize that women may have different symptoms of heart disease (atypical symptoms). These include nausea, shortness of breath, fatigue, dizziness, chest tightness rather than pain, or having pain in other locations such as the back, arm, jaw, or stomach.
Because these symptoms are less dramatic and less specific, there may be delays in recognizing the problem or the problem may be unknowingly ignored. Growing awareness that these symptoms may be due to heart disease also has helped to identify other patients, such as those with diabetes, who may not present with classic chest pain. Still, chest pain is the most common presentation of acute heart disease in women.
Awareness and Recognition—Patients and Doctors
Over the last several decades, there has been a growing awareness of the importance of heart disease in women. It is beneficial to recognize that heart disease is possible and common in both men and women for many reasons.
- Being aware of the signs and symptoms, whether typical or atypical, can help patients pay attention to whether they are experiencing symptoms and report them to their doctors.
- Increased awareness can help patients and doctors work together on lifestyle changes such as smoking cessation, heart-healthy diets, active lifestyles, and diabetes control.
- Correctly identifying, diagnosing, and managing heart disease early can lead to better outcomes, including quality of life and life expectancy.
Awareness that heart disease is the leading cause of death in women has increased over time. An awareness study conducted by the American Heart Association showed that in 2012, 56% of women correctly identified cardiovascular disease as their leading cause of death, compared to 30% in 1997. However, recognition of atypical heart-related symptoms such as nausea, fatigue, or chest tightness was still low.
Fortunately, advanced diagnostic tests and therapies for treatment of heart diseases, along with increased awareness, have led to lower death rates for men and women.
For more information, visit Adult Heart Disease.
The opinions expressed in this article are those of the author and do not necessarily reflect the views of The Society of Thoracic Surgeons.

