Chest Wall Tumors
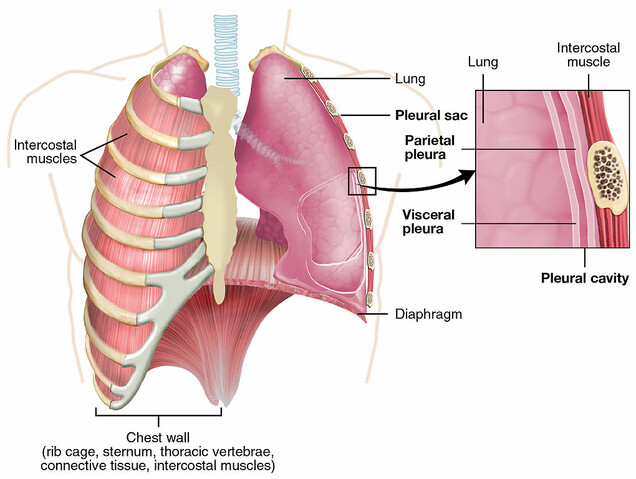
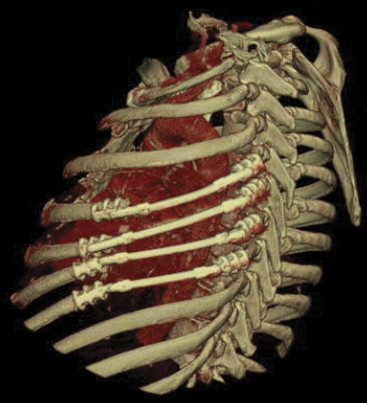
The chest cavity—which houses the lungs, heart, and other vital body parts—is a bone and muscle cage that is framed by the sternum (breastplate), spine, and ribs. The wall of the chest cavity provides rigid protection for your heart, lungs, and liver, but also is flexible to aid in respiration. It is made up of structures, including the rib cage, diaphragm, and abdomen. Like any other part of your body, your chest wall is susceptible to tumors.
Cells are the building blocks that make up the tissue and organs in your body. Old or damaged cells usually die and new cells take their place. But sometimes, the process goes wrong or a single cell starts to grow uncontrollably until it becomes a mass of tissue called a tumor.
Sometimes, tumors are non-cancerous (benign) and are not life threatening; other times, the tumors are cancerous (malignant) and can invade surrounding tissues or spread to other areas of the body.
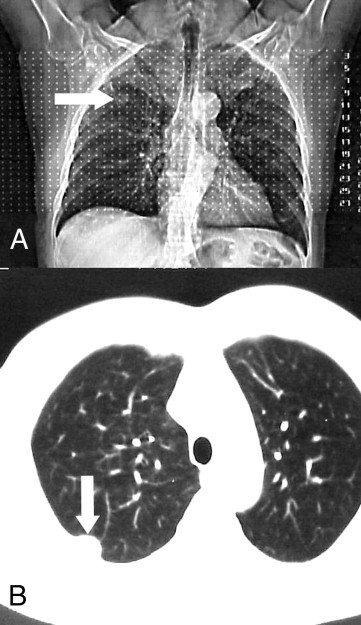
Chest x-rays can show whether or not you have an abnormality in your chest wall; however, x-rays are usually unable to distinguish benign tumors from malignant tumors.
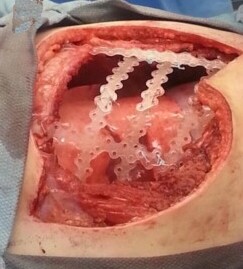
As with any surgery or procedure, there are risks involved.