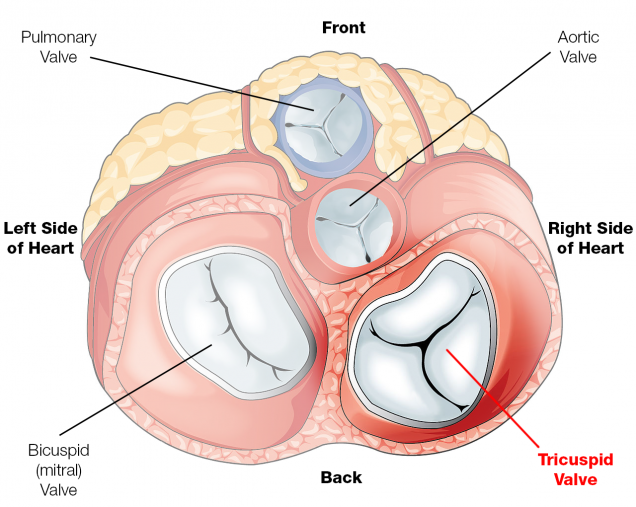
Tricuspid Valve Disease
The tricuspid valve is one of the two main valves on the right side of your heart. Normally, the tricuspid valve has three flaps (leaflets) that open and close, allowing blood to flow from the right atrium to the right ventricle in your heart and preventing blood from flowing backward.
Tricuspid valve disease occurs when the tricuspid valve doesn’t work properly. In some cases, the tricuspid valve is narrowed and doesn’t allow enough blood to pass through into your right ventricle (stenosis).
In other cases, the valve doesn’t close tightly enough, allowing blood to leak backward into the right atrium (regurgitation).
Tricuspid valve disease is not nearly as common as mitral or aortic valve disease. It is sometimes seen in combination with other valve diseases, such as mitral valve regurgitation.
While most people who undergo tricuspid valve surgery have a full recovery, potential complications include bleeding, infection, blood clots, irregular heart rhythm, or heart attack.